
Background of VRT
Virtual Reality Therapy
VR systems consist primarily of a computer setup and VR headset; however, chairs, gloves, and sensors are additional accessories that enhance the overall experience. These accessories transmit various physical sensations through haptic feedback systems. Virtual Reality Therapy (VRT) involves utilizing Virtual Reality (VR) technology to provide therapy by immersing patients in manageable and frequently engaging virtual settings. (Ali Adjorlu, 2024). VR is characterized by three fundamental attributes – immersion, a feeling of presence, and the ability to interact (Sokołowska, 2024). These attributes come together to support the core of VR, which engages participants in the interactive generated worlds of computers. Sensory data is provided with the help of a head-mounted display along with specialized interface devices. These monitor head movements, enabling the visuals to adjust fluidly by tracking head motion, thus enhancing the feeling of immersion (Maples-Keller et al., 2017).

Exposure therapy is the primary function regarding therapy, primarily due to the near-immediate recreation of real-world settings which helps to ensure a higher reproducibility (Bell et al., 2020). Virtual Reality Therapy (VRT) provides a safe, controlled environment for individual patients that can be adapted by therapists in real time based on the patient’s response. One of its key strengths lies in its immersive aspect and the gradual effects that occur over multiple sessions (Hembree et al., 2003). Patients adapt and learn behavioral skills to be able to prepare themselves when confronted with fear stimuli upon returning to the real world (Carl et al., 2019). The practice itself has been proven effective with various mental health conditions, and is viewed as a potential solution (Bell et al., 2020).

Traumatic experiences often cause individuals to associate specific mental images, sounds, thoughts, situations, physical symptoms, objects, and bodily sensations with that traumatic event and those are usually called fear stimuli (Abramowitz et al., 2011). Despite the fear stimuli present in these immersive environments, it is considered safe to undergo Virtual Reality Therapy as the patients are being guided and supervised by the therapists, monitoring any changes in behavior and patient response to the virtual scenario over time. However, as effective as it can be, patients still may refuse treatment or drop out of Virtual Reality Therapy, especially when exposed to their fear stimuli for periods of time (Deacon et al., 2013). It however has also been shown to provide benefits to patients suffering from post-traumatic stress disorder (PTSD), by giving patients a platform to be exposed and pull away from the stressor (Park et al., 2019).

Virtual Reality Therapy is an interactive form of therapy that collects information from the user’s sensory system while the VR glasses display a replication of the user’s specific experience with the fear stimuli present (Diemer et al., 2015). In real-time, the user or patient’s position and head movement behaviours are recorded with the help of a head tracking system placed on them (Wilczyński et al., 2016). These are usually done to accommodate those with anxiety disorders. When treating agoraphobia and social phobia, it becomes effective in multiple short sessions of at least 15 minutes or longer, 45 to 180 minutes. It’s noted that it’s effective in treatment when there’s no other pre-existing mental health condition that might affect the immersion or the interaction in the virtual world scenario (Meyerbroeker et al., 2013). The first study to investigate the effectiveness of VR therapy was Rothbaum et al., who tested the efficacy by treating acrophobia in college students; it was proven to have mitigated their fear of heights.

VR and Traditional Therapy
Traditional forms of exposure therapy, particularly cognitive-behavioral therapy (CBT), have been the standard for the treatment of anxiety as they have been known to significantly reduce the symptoms of the patients (Wolitzky-Taylor et al., 2008). When integrating the cognitive reframing strategy and exposure therapy, the treatment improved significantly than CBT alone (Norton & Price, 2007). Exposure therapy is grounded in the Emotional Processing Theory as the stimuli trigger fear and trauma in each person who has undergone a traumatic experience (Foa & Kozak, 1986).
In comparison, Virtual Reality Therapy (VRT) is a new form that is flexible and is able to tailor to the individual needs in their specific situations. This is due to the VR’s ability to manipulate the immersive scenario based on the patient’s set of fear stimuli that can be used to replicate the settings and environment as closely as possible. As it is new, there are still some hindrances to the patients as they may experience motion sickness, and derealization that results in conflicts when interacting with their therapist after each session with the VR (Benbow & Anderson, 2019).

Furthermore, Virtual Reality Therapy has its fair share of pros and cons. Examples of its benefits include convenience, reduced stigma, and much more. When discussing how such stigma can be reduced, Virtual Reality Therapy can remove a good number of the negative feelings associated with attending an in-person therapy session. On the other hand, the limitations of that kind of therapy include reliance on technology, and the lack of privacy (Ko, 2024). The main selling point of Virtual Reality Therapy is the personalization and ability to manipulate the environment with the relevant factors or variables tailored to the patient and the capability to interact with objects within the system. This eliminates the typical need to imagine or hire actors to replicate a scene for the patient. Despite these setbacks, it’s still considered a more convenient and safer alternative method of exposure therapy that’s adjustable. It provides an opportunity for its standardization of usage for the duration and exposure of patients.
Application of VR in Therapy
Treatment of Anxiety, PTSD, Phobias, and Other Illnesses.
With the use of VR and its recent innovations, it is now entirely possible to gather all the relevant data in real time. Included software are monitors for eye-tracking, heart rate, and skin conductance. All of which are typical physiological indicators of psychological states such as fear. Additionally, other centers have begun to process the integration of biosensors such as electroencephalography (EEG) to make more accurate assessments (Selaskowski et al., 2024). Mühlberger et. al, in particular, have developed a VR-delivered behavioural avoidance test (VR-BAT) to automatically collect heart rate, skin conductance, rating of discomfort, and stimulus-approach distance in order to assess the current impact of specific phobias.
Anxiety, post-traumatic stress disorder (PTSD), and specific phobias are among the most common and disabling mental health conditions today. They often develop after individuals are exposed to intense stress or trauma and can significantly interfere with daily functioning. Anxiety is generally characterized by persistent worry and fear that is difficult to control, while phobias involve intense, irrational fears of specific objects or situations. PTSD, on the other hand, can develop after a traumatic event and involves symptoms such as intrusive thoughts, flashbacks, hypervigilance, and avoidance of trauma-related cues (Carl et al., 2019; Parsons & Rizzo, 2008).
The outcomes of these disorders are often serious. For instance, individuals may struggle with maintaining personal relationships, experience academic or occupational difficulties, and have a decreased overall quality of life. Anxiety disorders and PTSD are also frequently comorbid with other mental health problems like depression, which compounds the psychological burden experienced by the individual (Fodor et al., 2018). Emotional avoidance, hyperarousal, and fear generalization are common coping responses that further reinforce the problem and prevent recovery.
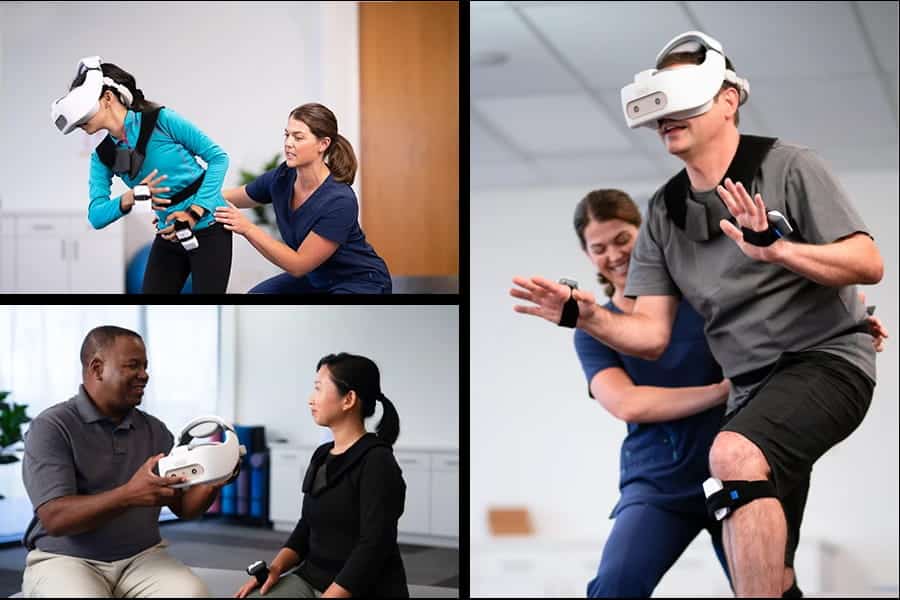
Virtual Reality Therapy (VRT) is a relatively new but promising form of treatment that addresses the challenges and inadequacies of traditional therapy, particularly when patients are reluctant or unable to face feared stimuli in real-world settings. Virtual Reality Therapy allows individuals to confront their fears in a controlled and customizable virtual environment with multi-sensory stimulation. Its computer-generated nature gives the opportunity for precise parameters to match patient preferences, not limited to frame rate, resolution, and design features. With these features, comes the phenomenon of “uncanny valley” where characters or features don’t feel human-like; giving a feeling of disgust or revulsion. This can be tackled by opting for more stylistic decisions creatively, as more stylized avatars tend to be easier to accept due to their lack of intentional lifelike movement (Bell et al., 2020).
In a meta-analysis conducted by Carl et al. (2019), Virtual Reality Therapy was observed to be highly effective in treating anxiety-related disorders, with outcomes comparable to those in vivo exposure therapy. The patient’s exposure to triggers or cues needed emphasizes the importance of customization in proving the effectiveness of the therapy (Bell et al., 2020). Similarly, Fodor et al. (2018) found that Virtual Reality Therapy produced significant improvements in symptoms of both anxiety and depression across a variety of clinical populations. Parsons and Rizzo (2008) further emphasized that Virtual Reality Therapy is especially useful for treating phobias, as the virtual environment can simulate specific feared situations with high realism and safety.
Virtual Reality Therapy has also been applied to the treatment of PTSD. According to Rizzo et al. (2020), virtual exposure significantly reduced PTSD symptoms when compared to control groups, indicating its strong potential as a therapeutic intervention for trauma-related disorders. Carl et al. (2019) also concluded that Virtual Reality Therapy is effective for PTSD treatment based on their large-scale analysis of randomized controlled trials. Furthermore, van ’t Wout‑Frank et al. (2024) explored the use of Virtual Reality Therapy in combination with transcranial direct current stimulation (tDCS) and noticed that it helped veterans with PTSD experience reduced anxiety and improved emotional regulation. The additional usages of VR apply to autistic or schizophrenic patients in helping to improve their social behaviour, showing that it also helps moderate Alzheimer’s disease through cognitive reserve and training (Park et al., 2019).
Obstacles Experienced
Despite promising findings, several challenges remain. Much of the PTSD research using Virtual Reality Therapy focuses on military populations, particularly veterans, so further studies are needed to assess its effectiveness in civilian populations (Rizzo et al., 2020). There is also variability in study methods and sample sizes across current literature, which makes it difficult to generalize findings. Moreover, there is limited data on the long-term effects of Virtual Reality Therapy, as many studies do not assess outcomes beyond six months (Fodor et al., 2018). Finally, combining Virtual Reality Therapy with other treatments such as pharmacological aids or brain stimulation techniques like tDCS may increase its therapeutic potential, however, more rigorous studies are necessary to validate these approaches (van ’t Wout‑Frank et al., 2024).
The reception to Virtual Reality Therapy has varying stances, with some claiming to reduce PTSD symptoms significantly while others countered that there are no differences to traditional treatments. However, it was later clarified that Virtual Reality Therapy patients experience the most success in relieving symptoms out of any other method. Additionally, there is a significant lack of consistency in the review compilation, being left primarily undefined and lacking clear usage of meta-analytical techniques to evaluate the efficacy of the treatment. Additionally, PTSD Patients are diverse in the challenges and experiences faced, however, the majority of reviewed subjects were combat-traumatized war veterans, and this factor lowers the credibility of effectiveness claims when it comes to PTSD.

The wide range emphasized in clinical VR research and experimentation complicates the study conduction and result collection, as experts from fields relating to computer science and clinical research are often required. Depending on its personalized nature, technical experts on the team may create complex scenarios that may appear as unbelievable to clinical mental health experts. The process of both development and approval from both fields makes it tedious and tight to organize. Due to this nature, it results in tight deadlines and frequent compromises that keep the research from meeting the minimum requirements for publication (Selaskowski et al., 2024).
Despite its supposed accessibility, VR programs intended for this purpose are commercially unavailable with a lack of proper infrastructure and training in clinical care for this device. The cost of adopting new technology can reach 400 dollars, for one set of the most recent version of the Oculus Quest. It’s challenging to maintain due to requiring constant software and hardware updates. Lastly, there are health concerns involved, ranging from dry eyes to VR sickness. Dry eyes occur from long and constant exposure to its very hot display and constant blue light. Another issue that comes up is its potential to be stressful to patients, or risk developing
addictions similar to that of online addiction (Park et al., 2019). Finally, genuine human contact appears to be preferred over machine usage to more vulnerable people (Selaskowski et al., 2024).
Rehabilitative Capacity of VR/VR Therapy
The simulative aspect remains, with research showing that participants experience virtual environments similarly to their real-life counterparts. It’s known to produce live emotional responses the same way, eliciting behaviours that align with standard expectations. Contrarily, patients who experience higher levels of paranoia have been shown to express detachment from the virtual environment (Bell et al., 2020).
The success of a client’s recovery in rehabilitation is closely linked to their perception of how positive their relationship with their therapist seems (Horvath & Symonds, 1991). Studies have highlighted the significance of verbal and non-verbal communication, especially in informal conversations where the therapist shares their own experiences, emotions, and opinions to strengthen their bond with their patient. The therapeutic alliance (TA) is further supported in Virtual Reality Therapy (VRT) where the primary purpose is to guide patients who have Acquired Brain Injury (ABI) during their sessions. This results in patients being more motivated and engaged in their recovery with the integration of VR therapy (Pinto et al., 2012).
A new method designed to be adaptive to the patient’s needs and facilitate the collaboration between therapist and patient. Communication is further supported through visual, haptic, or audio cues provided by the immersive nature of the VR. Additionally, it is a preferred method to those who rehabilitate with their upper limb because aside from better motivation and engagement (Aderinto et al., 2023), it directly helps with their cognitive function and task-specific learning, making it more effective than conventional therapy methods in certain cases (Aida et al., 2018).

Applied Theories in Research
Emotional Processing Theory
Emotional Processing Theory establishes the concept of a fear structure: a memory network that forms when an individual experiences a traumatic event. This structure contains information from the event, not limited to; the fear-inducing stimuli, an individual’s behaviour and response to those stimuli, and the meanings attached to them. Therefore, a person would most likely avoid situations, places, or signs that would trigger traumatic memories (Foa & Kozak, 1986).
Virtual Reality Exposure (VRE) is a form of treatment designed to help a person gradually learn new coping mechanisms to confront and process traumatic memories and fear stimuli. This was done to assist those who have Post-Traumatic Stress Disorder (PTSD) through a recreation of the event with visuals, sounds, and even smell to make the patient engage with it (Rothbaum et al., 1995). However, research noted that there were no significant outcomes if the patients themselves weren’t able to emotionally engage in the virtual scenario. Although there were also reports of decreased symptoms, no major differences were found between VRE and Prolonged Exposure (PE) therapy.
Classical Conditioning Theory
Classical conditioning theory, first proposed by Ivan Pavlov, provides a useful framework for understanding how anxiety, PTSD, and phobias develop and persist. This theory posits that individuals learn to associate a previously neutral stimulus (such as a place or sound) with a traumatic or fear-inducing event. Over time, the neutral stimulus alone becomes capable of triggering the same fear response—this is known as a conditioned response (Parsons & Rizzo, 2008). For example, a person who experienced a car accident may begin to feel extreme fear or anxiety whenever they are near a vehicle, even in a safe context. The conditioned fear response is further reinforced when the person avoids the stimulus, as this prevents the brain from learning that the stimulus is no longer dangerous (Carl et al., 2019).
This theoretical framework is relevant to exposure-based therapies similar to Virtual Reality Therapy. According to classical conditioning principles, fear can be reduced through repeated exposure to the feared stimulus without the presence of a negative outcome. This process, known as extinction, is what makes Virtual Reality Therapy effective—it provides individuals with repeated, safe exposure to their triggers in a virtual setting, allowing them to “unlearn” the conditioned fear response. Parsons and Rizzo (2008) explain that Virtual Reality Therapy builds on techniques like systematic desensitization and flooding, both of which aim to reduce fear through controlled exposure. In Virtual Reality Therapy, these principles are applied in a virtual environment, offering a safe and flexible way to present anxiety-provoking stimuli at varying levels of intensity. Carl et al. (2019) support this view, noting that the customizable nature of Virtual Reality Therapy environments allows for graded exposure, which aligns closely with the gradual exposure techniques derived from classical conditioning theory.
Moreover, by using virtual simulations, therapists can precisely control the intensity and duration of exposure, ensuring that the patient stays engaged and that the therapy option is tailored to their needs. This controlled setting minimizes the chances of retraumatization and increases the likelihood of successful fear extinction. The incorporation of Virtual Reality Therapy into treatment thus represents a modern adaptation of classical conditioning theory, enhancing its application with the use of immersive technology.

